New Delhi: India’s healthcare system may be expanding in reach and ambition, but its gains remain uneven, exposing persistent structural inequities across regions and sharply divided economic strata. The latest national survey points to a clear shift: more Indians are seeking care, more are covered by insurance, and more are accessing public health services at lower cost. Yet beneath these gains lies a more complex reality — one where affordability gaps, rising non-communicable diseases, and dependence on private providers continue to test the government’s repeated promise of universal healthcare.
Access has improved, and financial protection has widened, but the burden of healthcare spending has not disappeared. It has merely shifted and, in some cases, deepened.
This was revealed in the latest survey on Household Social Consumption on Health by the National Statistical Office (NSO), which covered 1,39,732 households across rural and urban India.
Rising Access, Changing Behaviour
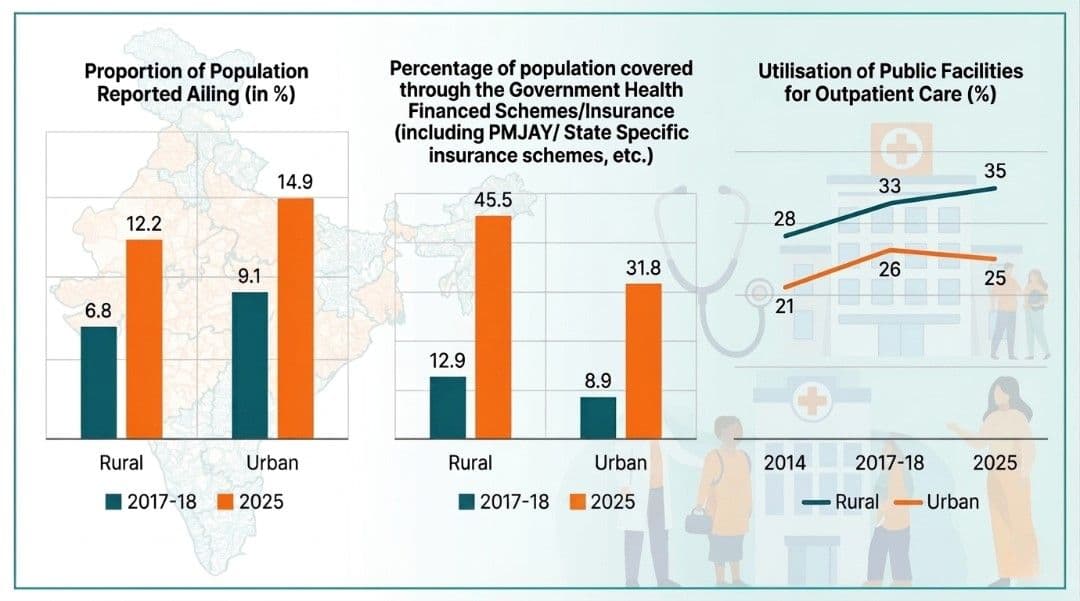
One of the most striking findings is the sharp rise in health-seeking behaviour. The proportion of population reporting ailments (PPRA) has nearly doubled since 2017-18, reaching 12.2% in rural areas and 14.9% in urban India. This increase does not necessarily signal worsening health; rather, it reflects greater awareness, improved access, and a willingness to seek treatment.
This shift has been supported by sustained public investment in healthcare infrastructure, from primary care centres to tertiary hospitals. The expansion of Ayushman Arogya Mandirs and the scaling up of free drugs and diagnostics initiatives have brought services closer to communities, particularly in rural areas.
At the same time, the epidemiological profile of the country is changing. Infectious diseases are declining, while non-communicable diseases such as diabetes and cardiovascular conditions are on the rise. This transition demands a healthcare system that is not just reactive but preventive—something the report suggests is still a work in progress.
Affordability up, Fault Lines Persistent
The report highlights encouraging trends in affordability. The median out-of-pocket expenditure (OOPE) per hospitalisation stands at ₹11,285, with public facilities significantly lowering this burden to around ₹1,100 in more than half of cases. For outpatient care in public facilities, the median OOPE is effectively zero, underscoring the impact of government-backed free services.
Insurance coverage has also expanded dramatically. Government-financed health insurance schemes now cover 45.5% of the rural population and 31.8% of the urban population, more than tripling over the past few years. This expansion marks a significant step toward financial risk protection.
However, averages conceal disparities. A small number of high-cost cases continue to push up overall expenditure, and the reliance on private healthcare remains a major driver of financial stress. Nowhere is this more evident than in childbirth costs. Deliveries in private hospitals cost nearly 16 times more than in government facilities, with median expenses of ₹32,000 compared to just ₹801 in public institutions.
Despite public sector improvements, the share of childbirths in private hospitals is rising, particularly in urban areas. This trend suggests that trust, perceived quality, and accessibility still tilt many patients toward private providers, often at a steep financial cost.
Challenges Remain
The utilisation of public healthcare facilities is slowly increasing, especially in rural India, where outpatient usage has risen from 28% in 2014 to 35% in 2025. This reflects growing confidence in public systems, aided by expanded services and reduced costs.
Maternal and child health indicators also show steady progress. Institutional deliveries have become nearly universal, reaching 95.6% in rural areas and 97.8% in urban India. Government schemes promoting safe motherhood have clearly delivered results.
Yet gaps remain. Post-natal care, while high, still lags behind ante-natal coverage, pointing to weaknesses in continuity of care. More broadly, the system continues to struggle with balancing scale and quality, especially as demand rises.
Stress on System
What the data also hints at, though less explicitly, is the emerging stress on the system from this very expansion. As more people enter the formal healthcare net, capacity constraints — from doctor availability to diagnostic turnaround times — are likely to intensify unless investments keep pace.
The widening insurance coverage, while critical, may also inadvertently reinforce private sector dependence if public facilities are unable to absorb rising demand. This risks creating a two-speed system, where those who can navigate or afford private care continue to do so, while the rest depend on an overstretched public network.
Equally concerning is the limited evidence of financial protection in cases requiring specialised or long-term care, particularly for non-communicable diseases. Chronic illnesses demand sustained expenditure, and even modest out-of-pocket costs can accumulate into significant financial strain over time. Without stronger primary care integration and continuity mechanisms, the system may struggle to manage this growing burden effectively, say healthcare experts.

