New Delhi: For decades, the global health community has pointed to the steady decline in maternal mortality as one of the great success stories of modern medicine. However, a major new study published in The Lancet Obstetrics, Gynaecology & Women’s Health suggests that this era of rapid progress may be coming to a close.
While the total number of women dying from pregnancy-related causes has fallen significantly since 1990, the pace of improvement has slowed dramatically in recent years, leaving many nations, including India, struggling to bridge the final gap in maternal safety.
The scale of the challenge remains immense. The study estimates that in 2023, approximately 240,000 women died globally due to pregnancy- and childbirth-related causes. This staggering figure means that maternal deaths now account for 5.5% of all deaths among women and females aged 10-54 years.
The researchers noted in their assessment of the current landscape that “maternal mortality has decreased globally in the past three decades; however, mortality remains high in some locations and progress has plateaued or reversed in others.”
The Indian Paradox
India serves as perhaps the most significant example of both the triumphs and the "unfinished work” described in the report. On the one hand, the country’s historical achievements are undeniable. Maternal deaths in India have fallen sharply from an estimated 1.19 lakh in 1990 to 36,900 in 2015, and further down to 24,700 in 2023.
This downward trend is mirrored in the Maternal Mortality Ratio (MMR) — the number of maternal deaths per one lakh live births. India’s MMR has declined from 508 in 1990 to 116 in 2023. This represents a monumental shift in the safety of childbirth for millions of women. Yet, despite these gains, India remains among the highest-burden countries globally. Alongside Nigeria, Pakistan, Ethiopia, and the Democratic Republic of the Congo, India still accounts for a disproportionate share of the world’s maternal deaths.
The study highlights that while the early years of the millennium saw rapid gains, the momentum has since flagged. During the Millennium Development Goal (MDG) period from 2000 to 2015, global maternal deaths declined at an annualized rate of 3.6%. However, in the early Sustainable Development Goal (SDG) era (2015-2023), this rate of decline slowed to 3.0%.
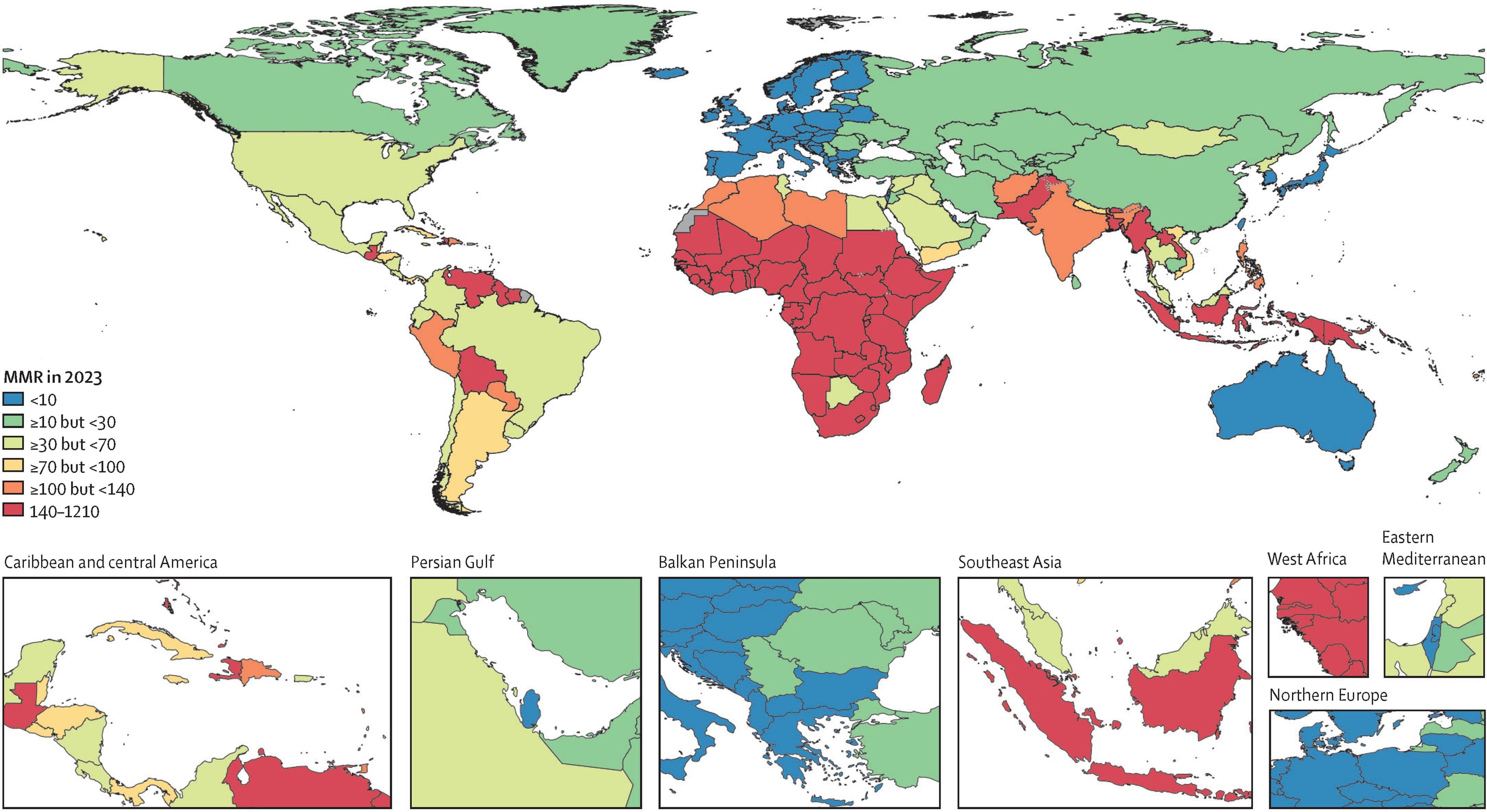
Regional Divergence
The global stagnation is not uniform, but rather a collection of regional stories. While some areas continued to improve, others saw their progress wiped out by emerging threats. The report emphasizes that the global MMR of 190.5 in 2023 is still more than double the international target. The study’s authors were blunt in their evaluation of the current trajectory, saying, “Global MMR in the most recent year of estimation was more than double the SDG target... 104 of 204 countries and territories have yet to meet the SDG goal of fewer than 70 maternal deaths per 100 000 livebirths.”
The COVID-19 pandemic acted as a brutal disruptor. In regions like Latin America, the Caribbean, and high-income North America, maternal deaths actually rose in 2020 and 2021. These spikes were often driven by "indirect" maternal deaths — cases where the physiological stress of pregnancy exacerbated the severity of a COVID-19 infection — rather than a failure of obstetric care itself. In many data-rich locations, the health systems’ ability to manage standard complications like haemorrhage remained robust, but they could not compensate for the added risk the virus posed to pregnant women.
Need for New Approach
The data confirms that the primary biological causes of maternal death remain tragically consistent. Maternal haemorrhage and hypertensive disorders continue to be the top two sub-causes of death globally. In 2023, haemorrhage accounted for 21.7% of deaths, while hypertensive disorders followed closely at 20.1%.
However, the report suggests that clinical interventions during labour are no longer enough. To reach the next level of safety, health systems must look at the “continuum of care” that begins before conception and extends long after delivery. This includes addressing malnutrition, providing better access to family planning to prevent high-risk or unwanted pregnancies, and expanding primary care in the full year following childbirth to catch “late” maternal deaths.
Age also plays a critical role in risk profiles. While the largest absolute number of deaths in 2023 occurred among women aged 20-24 (approximately 49,000 deaths), the highest ratio of mortality was found among women aged 50-54, where the MMR reached a staggering 2,150 per one lakh live births. This disparity underscores the heightened risks faced by older mothers, often due to pre-existing medical conditions that are exacerbated by pregnancy.
Call for Resilience
One of the most concerning findings in The Lancet report is the persistence of “data deserts”. The regions with the highest burden of maternal deaths are often the ones with the least reliable reporting systems. In 2023, eight countries still had no direct input data for maternal mortality at all. Without accurate, timely data, health officials are essentially flying blind, unable to identify which interventions are working and which areas are falling behind.
As the 2030 deadline for the SDG looms, the report serves as a warning. The era of “easy” gains in maternal health may be over. Future progress will require more than just building hospitals; it will require building resilient health systems capable of weathering global pandemics while providing equitable care to the most vulnerable women.
“Emerging global health threats such as COVID-19 present an additional barrier to meeting and sustaining SDG targets... the stagnation of global progress highlights the need for health-care systems to strive to provide high-quality, accessible care while remaining agile,” the report says.
For India and the rest of the high-burden world, the message is clear: the sharp declines of the 1990s and 2000s were a beginning, not an end. To finish the work and reach the target of fewer than 70 deaths per one lakh live births, a renewed, data-driven commitment to women’s health is now a matter of global urgency.

