New Delhi: As health officials race across continents to trace cruise passengers, isolate suspected carriers, and prevent further spread, the latest hantavirus outbreak has triggered a wave of global anxiety reminiscent of the early days of past international health scares.
Airports have quietly intensified monitoring, emergency response teams have been activated in multiple countries, and epidemiologists are scrambling to determine whether the virus could evolve into a wider public health crisis.
The discovery of a rare hantavirus strain capable of limited human-to-human transmission has amplified fears, especially after fatalities linked to the outbreak began surfacing across international jurisdictions. While authorities insist the threat remains contained, the rapid mobilization of global surveillance systems has placed governments and healthcare agencies on high alert.
A renewed global focus on hantavirus has emerged after a deadly outbreak linked to the Dutch cruise ship MV Hondius triggered international health alerts, passenger tracing operations, and emergency coordination involving multiple countries. While global health authorities insist that the situation is not comparable to the COVID-19 pandemic, the outbreak has nevertheless exposed vulnerabilities in disease surveillance, travel monitoring, and outbreak communication systems across continents.
The current scare began after several passengers aboard the expedition cruise vessel developed severe respiratory illness during a South Atlantic voyage. The ship had travelled through remote ecological zones including Antarctica, South Georgia, Tristan da Cunha, Saint Helena, and Ascension Island before health authorities were notified. By early May 2026, the World Health Organization confirmed multiple hantavirus infections, including fatalities and several suspected cases.
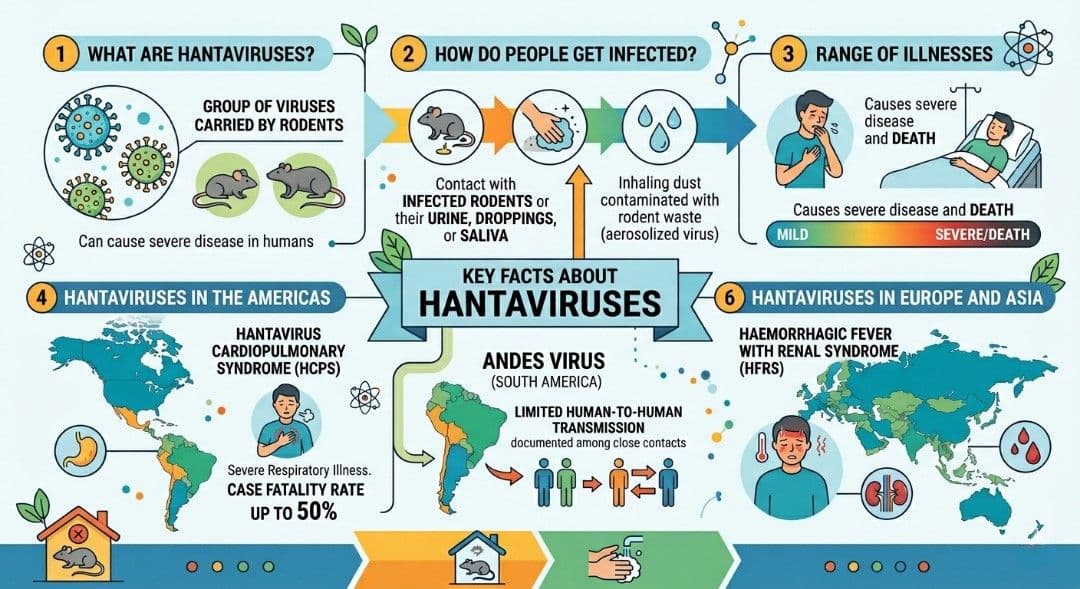
Scientists believe the outbreak is linked to the Andes strain of hantavirus, one of the rare variants capable of limited human-to-human transmission. Most hantaviruses spread primarily through exposure to infected rodent urine, droppings, or saliva. Humans generally contract the disease by inhaling contaminated dust particles in enclosed or poorly ventilated spaces.
One of the most discussed aspects of the outbreak has been the emergence of what epidemiologists are informally calling ‘POINT ZERO’ — the earliest identified infection source linked to the cluster. According to international investigators, the probable POINT ZERO case involved a passenger who had travelled through Argentina, Chile, and Uruguay before boarding the ship. Health authorities suspect exposure occurred during visits to bird-watching regions inhabited by rodents known to carry the Andes virus. WHO investigators believe the virus was likely introduced onboard by this initial infected traveller before limited transmission occurred among close contacts during the voyage.
The World Health Organization has repeatedly attempted to calm fears of a large-scale pandemic. WHO Director-General Tedros Adhanom Ghebreyesus stated that while the incident is serious, the overall global public health risk remains low. WHO epidemic preparedness expert Maria Van Kerkhove emphasized during a media briefing that “This is not COVID. This is not influenza.” The organization clarified that hantavirus spreads very differently and does not transmit easily in casual community settings.
The WHO advisory currently focuses on aggressive contact tracing, isolation of symptomatic individuals, laboratory surveillance, and international cooperation among affected nations. The agency has urged countries to monitor passengers who may have disembarked before the outbreak was identified. WHO is also developing operational guidance for safe disembarkation and international travel procedures connected to the outbreak response.
Countries Take Precautions
Twelve countries have already been formally alerted by WHO because passengers from those nations disembarked at Saint Helena during the voyage. These countries include Canada, Denmark, Germany, the Netherlands, New Zealand, Saint Kitts and Nevis, Singapore, Sweden, Switzerland, Türkiye, the United Kingdom, and the United States. Additional monitoring has also involved South Africa due to medically evacuated passengers and potential exposure during international flights.
Several governments have activated precautionary health protocols in response to the scare. The Netherlands implemented strict isolation procedures for passengers returning from the vessel and coordinated medical evacuation measures with public health agencies. Dutch authorities stated that quarantine and onboard infection-control systems had already been activated even before the specific hantavirus strain was confirmed.
South Africa intensified hospital surveillance after receiving critically ill evacuated patients from the ship. Local authorities began tracing airline passengers and healthcare contacts linked to infected travellers. Laboratories in the country played a crucial role in confirming the hantavirus diagnosis through PCR testing.
European health agencies, including the European Centre for Disease Prevention and Control, launched coordinated epidemiological assessments across multiple EU states. Passenger monitoring systems were activated in countries whose citizens had travelled aboard the ship. Authorities also began evaluating possible secondary exposures among family members, healthcare workers, and airline contacts.
The United States and Canada increased surveillance for travellers returning from affected regions and initiated public health observation for individuals potentially exposed to infected passengers. Some U.S. state health departments confirmed monitoring asymptomatic travellers who had returned home after disembarking from the cruise.
Singapore and several European nations reportedly strengthened airport health coordination and advised clinicians to remain alert for unexplained respiratory illnesses accompanied by rodent exposure history or recent international travel linked to the outbreak.
Despite the intense media attention, infectious disease experts continue to stress that hantavirus remains rare globally. WHO data indicates that hundreds — not millions — of cases are typically reported annually across affected regions. Most outbreaks remain localized and are linked to environmental exposure rather than sustained human transmission.
Medical experts note that hantavirus symptoms often begin with fever, fatigue, muscle aches, nausea, and headaches before rapidly progressing in severe cases to respiratory distress and pneumonia. Because early symptoms resemble influenza or other viral illnesses, diagnosis can be delayed. Severe forms such as Hantavirus Pulmonary Syndrome can become life-threatening if treatment is not initiated quickly.
The outbreak has also revived debate about the world’s readiness for future infectious disease emergencies. Public health specialists have warned that misinformation surrounding hantavirus is spreading faster than the virus itself in some regions. Experts fear that social media panic, combined with declining trust in public health institutions after COVID-19, could complicate future outbreak responses even when risks remain relatively contained.
At present, WHO maintains that the hantavirus outbreak is expected to remain limited if countries continue implementing containment measures and international coordination. The organization has nonetheless warned that additional cases may still emerge as contact tracing and testing continue across multiple jurisdictions.

